Posted
Categories: Patient Voice Mail, Working Together for Better Health Care
Interior Health is making improvements to medical imaging across the region to improve the quality of care, including access to services, and to explore innovative opportunities into the future.
Interior Health leads Lynne James, Project Lead, Medical Imaging Strategy; Kevin Peters, Director of Medical Imaging; and Dorte Kargut, Administrative Assistant, reached out to the Patient Voices Network (PVN) to engage patient partners to learn from their experiences. Their goal was to hold a one-time focus group to seek input into their five-year service plan.
The invitation was shared through our communication channels in January and February 2022 and we had an overwhelming response with almost 20 patient partners stepping forward. The response was so great that Lynne decided to split the group in half and offer two 90-minute virtual focus groups as well as one-to-one interviews with three others.
When we asked PVN patient partner Richard Delaney why he joined the group, he responded, “I wanted to give back to the health care system that we all own and are proud of.”
The following six themes emerged from the focus groups and written submissions:
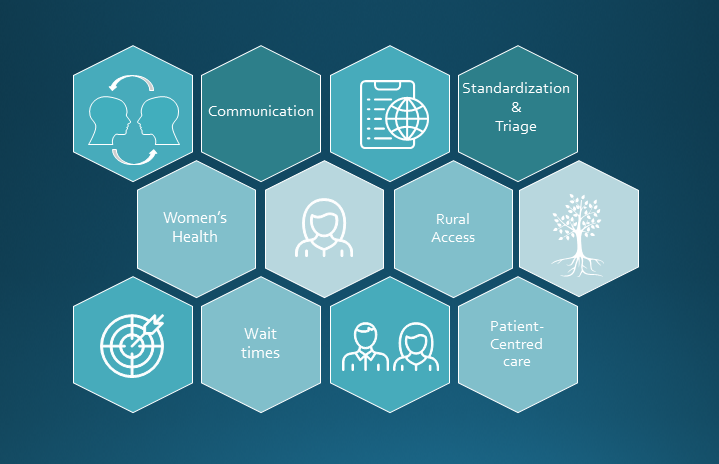
Gaps in communication before and after imaging scans were identified by the participants. For example, patients may not hear back for months after the requisition is sent in from the health care provider and patients are left wondering if the requisition was lost. One patient partner described the wait as being “off in the wilderness waiting”. After the scan, patient partners without a family doctor expressed the challenging nature of not knowing who will follow up with their results.
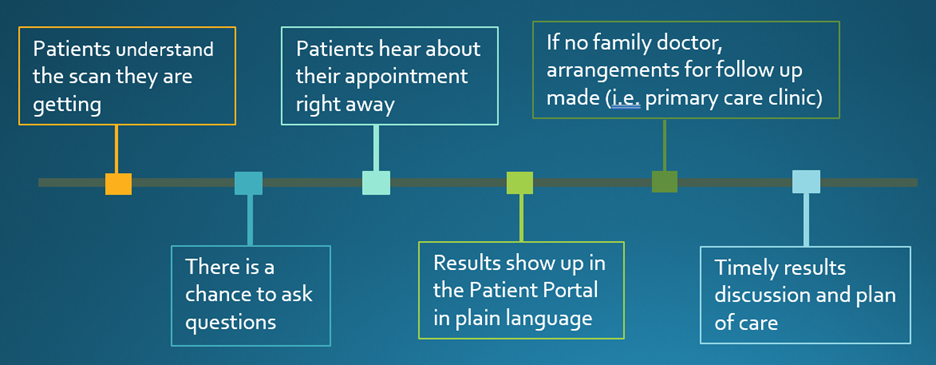
On the theme of “communication”, the vision for change also included the following:
From the theme of “rural access”, distance from service and mountain passes with severe weather were identified as significant barriers to accessing care. Patient partners shared that with travel, a single scan can take up to two days.
And from the theme of “patient-centred care”, participants shared that staff may not understand that Aboriginal patients may be distrustful of health care institutions as a result of systemic racism. This distrust is not only a barrier to equitable care but may also result delays in treatment.
The final report is still in development and will include tangible recommendations from these focus groups on various topics:
- Standardization of protocols and the use of artificial intelligence
- Streamlining the appointment booking process and improving communication about appointments with patients
- Improving access for people in rural and remote communities
- Reducing wait times and increasing transparency of wait times
Artificial intelligence in medical imaging can be used to support diagnosis and evaluation.
“The focus groups exceeded our expectations. The patient partners shared their experiences of medical imaging services in such a compelling way. They also provided so many practical ideas to help us improve our program. I was impressed!”
Lynne James, Project Lead, Medial Imaging Strategy
Kevin Peters, Director of Medical Imaging, said, “The stories, ideas, and feedback from the patient partners provided invaluable insights which helped shape the medical imaging service plan. We look forward to sharing updates with the focus group members as the plan is finalized.”
Author: Carol Stathers, Engagement Lead, BC Patient Safety & Quality Council


